CASE STUDY
Mr Ali
This case concerns a man with neurological and physical impairments in the aftermath of a stroke, who is cared for by his wife Mdm Siti, and by Enziroh, a foreign domestic worker. When Mr Ali’s home care plan falls apart repeatedly, what should hospital staff do differently?
These materials may be downloaded and copies may be made for teaching purposes, but not republished in part or whole elsewhere in electronic or print or any other medium. The National University of Singapore retains full copyright on these materials.

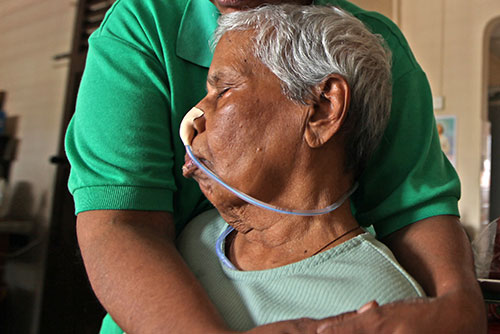 Before We Forget / Lien Foundation
Before We Forget / Lien Foundation
This case concerns a man with neurological and physical impairments in the aftermath of a stroke, who is cared for by his wife Mdm Siti, and by Enziroh, a foreign domestic worker. When Mr Ali’s home care plan falls apart repeatedly, what should hospital staff do differently?
Mr Ali
‘Take care, Mdm Siti. Please follow up with the clinic next week about your husband’s appointments.’
Ms Aisha, a medical social worker, has just completed Mr Ali’s discharge procedure from a community hospital; this was his third hospitalisation since his first stroke the previous year. After they have stepped away from the patient’s bedside, her colleague, Dr Ng, says, ‘I hope the discharge plan works this time.’
‘I know, I know,’ Aisha responded, ‘At least we persuaded the patient’s wife to hire a domestic helper. Mr Ali could be cared for in a nursing home, but the family was not open to that when I mentioned it. They have two daughters in KL and a son in Australia, but no one here. And they don’t want to spend more on other services, now that they’re paying for a maid.’
‘Well, we do what we can while they’re here, then we send them home and hope for the best. Okay, who’s next on the list?’
Eight weeks later, Mdm Siti once again wakes up in the middle of the night. She calls to Enziroh, an Indonesian domestic worker who now lives with Mr Ali and Mdm Siti in their four-room HDB government flat. They speak in Malay.
‘Enzi! Enzi! Wake up! Come quickly! The bed is wet again. We have to change his clothes and sheets. Help me lift him. Why must it always happen at this hour?’
‘Yes, Ma’am. Let me do. You are not well.’
‘He doesn’t want you to do it. Just do as I say. I am fine. Just a bit out of breath, I think because I have been waking up all these nights.’
Three weeks later, the members of a discharge team at an acute care hospital meet to discuss a pending transfer concerning Mr Ali.
‘Okay, let me review the notes. Mr Ali, aged 78, was admitted through the A&E five days ago. The admitting physician recorded that he was slightly dehydrated and also constipated. He had been discharged from a community hospital a few months ago, after his second stroke. As far as we know, he has never gone for physiotherapy – no transport, probably. He’s just been at home.’
‘His wife, Mdm Siti, aged 73, is the primary caregiver, and there’s a domestic helper. Mdm Siti has a few medical problems too – diabetes, uncontrolled hypertension – she could get a stroke herself. The physician who admitted Mr Ali recorded that the maid told one of the nurses that Mdm Siti was having trouble breathing. I asked Mdm Siti about that but she was annoyed and said the maid was wrong. I hope I didn’t get that maid into trouble.’
‘So it’s clear that Mr Ali needs to return to the community hospital to get some physio. Perhaps he can get some mobility back, maybe even use a walking frame. He needs help with personal care – bathing, toileting, dressing, making sure he eats.’
‘Well, he’s right back where he was a few months ago. It doesn’t sound like things are going to change at home once he’s discharged again.’
‘So, what should we do?’
Supporting older people and their caregivers at home
Commentary by Jacqueline Chin and Nancy Berlinger
How can community care services help families?
Services aimed at supporting ageing or chronically-ill Singaporeans in their homes may not, in reality, touch the lives of people who cannot afford to pay out-of-pocket for services, or cannot as yet foresee the ways in which everyday life changes after the onset of illness, disability, or frailty and dementia. In the aftermath of a second stroke, Mr Ali appears to have been confined to his flat for months, with a spouse who urgently needs respite, and a newly-employed foreign domestic worker in lieu of a nursing home placement.
Do Mr Ali and family caregivers know his condition and understand his prospects?
It is unclear how much Mr Ali, Mdm Siti, and Enziroh (Enzi) know about his condition or the realistic prospects for him to regain enough mobility to use a walking frame. These are important issues for each member of this household to understand. Professionals involved in Mr Ali’s care have a responsibility to have regular discussions with him and his caregivers to assess understanding of his condition, his current personal care needs, and the goals of physiotherapy for him.
Is community physiotherapy physically and financially inaccessible?
While Mr Ali will receive physiotherapy in the community hospital, another aspect of his care that is unclear is whether this household has access to physiotherapy in the community, or space in the home for home physiotherapy. If it is physically or financially impossible for Mdm Siti, even with a foreign domestic worker’s help, to attend to Mr Ali’s personal care and also bring him to physiotherapy appointments, that part of his care plan isn’t working as anticipated, and medical problems and suffering resulting from immobility are likely to continue to arise.
How can Mdm Siti gain respite and a care role that works?
Respecting Mdm Siti as a person means not simply reducing her to the role as a caregiver. This is also a practical matter as well as a question of respect: Mdm Siti is ageing herself, and the physical demands of her husband’s basic care are affecting her ability to attend to her own health. Advising or admonishing a person in Mdm Siti’s position about the importance of self-care does not solve this problem, and could be perceived as disrespectful or unrealistic by a caregiver who does not have local family members to turn to so she has time for her own needs.
The reasons for Mdm Siti’s earlier refusal of nursing home care on behalf of Mr Ali should be explored by the transitional care team and by the team who will care for him in the community hospital. If a nursing home placement is still not acceptable to this family, they may need help understanding that a home care plan that relies heavily on an ageing spouse is precarious, and could lead to a nursing home admission under crisis conditions if Mdm Siti’s own health fails. Asking Mdm Siti who, if anyone, helps her make difficult decisions, may provide professionals with greater insight into the role of the couple’s adult daughters in their parents’ lives: does Mdm Siti perceive that she is alone in coping with these immense challenges?
How can families and foreign domestic workers be better prepared to manage tensions in home care?
A home care plan that includes employing a foreign domestic worker, who is introduced into the household around the time of a hospital discharge, can be problematic in several ways. Even when a foreign domestic worker is trained to care for elderly people at home, the addition of a new person living in the household, as an employee, can increase rather than relieve tension. The person who tried to help both Mr Ali and Mdm Siti – Enzi, who conveyed her observation about Mdm Siti’s breathlessness to a hospital nurse – potentially put herself at risk when a hospital team member mentioned this concern to Mdm Siti.
When family caregivers are advised to hire a domestic worker as a live-in caregiver, respect for this person should be part of care planning. Whether or not a family has ever employed foreign domestic workers, the high-stress conditions of home healthcare are foreseeable. Providing appropriate training to foreign domestic workers, and to paid workers and family caregivers together, is one way of mitigating this stress and to demonstrate respect for caregiving work. Another way is helping employers and paid workers communicate and collaborate in the home, mindful that they may not share a language or be familiar with each other’s cultures.
How can healthcare professionals demonstrate shared responsibility for the care needs of people in the community?
It is important to acknowledge that high-stress situations typical of home care can lead to unrealistic expectations on caregivers as well as them being blamed unjustly. Developing home care plans that do not fail after the institutional supports of hospitalisation or transitional care are removed, and that can adapt to a chronically-ill or ageing person’s changing needs, are ways that professionals can demonstrate shared responsibility for the care needs of people in the community.
Close attention to practicalities, such as affordable transportation to physiotherapy or access to home care services that include medical, nursing, and social work professionals to supplement the work of family caregivers and domestic helpers, are structural ways to strengthen home care plans so that they ease burdens on caregivers. These approaches also ensure that caregivers at home have access to professional help before a crisis arises.
Citation
Commentary by Chin, Jacqueline and Berlinger, Nancy ‘Supporting older people and their caregivers at home’, in Chin, Jacqueline, Nancy Berlinger, Michael C. Dunn, Michael K. Gusmano (eds.), A Singapore Bioethics Casebook, vol. ii: Caring for Older People in an Ageing Society (Singapore: National University of Singapore, 2017), http://www.bioethicscasebook.sg.
The ethics of discharge planning
Commentary by Michael K. Gusmano and Nancy Berlinger
Should the hospital have done more to support Mr Ali and his caregivers? Hospitals are often under pressure to discharge patients. All healthcare systems, even those in wealthy societies like Singapore, face resource constraints. If hospital administrators and clinicians fail to discharge existing patients on a timely basis, this could delay care and could even result in avoidable death of patients waiting for admission.
The importance of developing a realistic plan for caregiving
As the discharge planning team member noted, Mr Ali was about to be discharged to a community hospital and then back home in which his caregiver was overwhelmed, and neither the caregiver nor the patient would have access to professional support. The last time Mr Ali was discharged from the community hospital, he failed to receive the physiotherapy and other follow-up care that may have prevented his health from deteriorating further.
This case presents a distressingly familiar scenario in ageing societies: a person who is experiencing serious, age-associated health problems – in this case, a series of strokes – that have impaired his ability to complete tasks of daily living; another person who is designated as the caregiver, and who is also ageing; yet another person or a series of people who are paid to help hold things together; still more people, who are paid to patch things up when the plan falls apart, to devise a new plan and hope for the best. It highlights the ethical challenges that arise when a hospital discharge is reduced to bed-clearing, or ‘pushing the patient home’, rather than preparing and supporting the reality of caregiving in the community. The hospital was about to discharge Mr Ali back to the community hospital and ‘hope for the best’, even though it seemed likely that this would result in the same problems.
Who is responsible for planning?
Who is responsible for developing a care plan, getting others to agree to it, and providing the sustained structural support that ageing, ill, or disabled people living at home may need? To what extent do members of the acute care hospital team have a responsibility to coordinate their discharge plan with members of the community hospital and/or community-based agencies that may be able to provide additional support?
Taking the responsibility question first: there is a built-in dilemma in transitional care, which is designed to meet the goal of preventing avoidable re-hospitalisation during a period of transition from acute hospital care to another setting, usually to a community hospital, followed by a discharge home. However, people who are chronically ill, or who are experiencing progressive, age-associated frailty, are not in transition from illness to health: they are, at best, aiming for stability. In this household, we glimpse a person who may be able to regain some physical capacities, but who cannot get himself to physiotherapy. This person currently relies on others for personal care, and is uncomfortable with some types of care, under some conditions: Mr Ali may object to a foreign domestic worker cleaning him at home, but may not object to a nurse performing the same care in the different setting of the hospital. How can the transitional care team, in the limited time available to them, help Mr Ali (whose cognitive capacity and ability to communicate is unclear) to express his concerns, as a person, and to adapt to his condition?
It is important for teams within hospitals to know about the settings to which patients are being transferred. Without knowing more about the environment in which their patients will live, it is impossible for clinicians to make appropriate transfer decisions or help families prepare for these transfers. Hospitals need to do a better job of acquainting clinicians with the realities of ‘home’ as a care setting. Hospitals and their staff have an obligation to address social, economic, and other factors that make discharges difficult. To do so, they must be aware of these factors, discuss these issues with patients and families, and help families arrange for appropriate care in the community.
Citation
Commentary by Gusmano, Michael K. and Berlinger, Nancy, ‘The ethics of planning discharge’, in Chin, Jacqueline, Nancy Berlinger, Michael C. Dunn, Michael K. Gusmano (eds.), A Singapore Bioethics Casebook, vol. ii: Caring for Older People in an Ageing Society (Singapore: National University of Singapore, 2017), http://www.bioethicscasebook.sg.
Discharge planning
Practice Perspective by Christopher Lien
Mr Ali has had a previous stroke and has ongoing problems with mobility, transfers, toileting, oral feeding, fluid intake, and probably has difficulty engaging in a routine that is meaningful to himself in the course of the day. He seems to have deteriorated in his function from the time he was first discharged from hospital. Not mentioned in the case history is whether Mr Ali is depressed (which can be treated) or the extent to which he is cognitively impaired (which may require specific skills and understanding to provide care that is effective and sustainable).
What is the current reality at home?
Mdm Siti, who is herself in frail health, seems stressed, somewhat torn and disorientated by the competing demands of caregiving. Both she and her domestic worker Enziroh don’t seem to be adequately equipped to set up a sustainable daily routine, or to address obstacles in their care for Mr Ali, such as in managing his oral and fluid intake, urinary incontinence, and constipation.
Effective problem-solving skills at home are key to crisis prevention, which in turn, reduce the risk of repeated admissions and unsuccessful discharges.
What realistic goals should we be aiming for?
An important functional goal is the maintenance of mobility and the adherence to a daily routine for Mr Ali. The ease with which he is able to get out of bed is determined by the extent of assistance he requires. However, the ability to involve Mr Ali himself as much as possible in all his movements is an important skill in his health maintenance. For this to happen, Mdm Siti and her domestic worker need a good understanding of stroke disease, its potential complications, and its rehabilitation. Psycho-social support for Mr Ali as he struggles with his debilitating and progressive disabilities would also help him be a more active partner in his care and recovery. Knowledge of the different options of care and available resources in the community can also help family members make appropriate choices.
What services are in place for the post-discharge care of Mr Ali?
Available resources from the Ministry of Health (MOH), Agency for Integrated Care (AIC), Ministry of Social and Family Development (MSF) and NTUC Health include hospital transitional care services, ongoing home-based rehabilitation, home nursing, hospital and community social workers, and cluster support to coordinate the access and delivery of multiple services. However, most of these services require out-of-pocket payments and family members are often disorientated by the multiple choices they have to make, and the multiple points of contact they have to access.
What resources are needed to devise a sustainable plan?
Effective post-discharge care requires a seamless system to facilitate partnership between health providers and family caregivers, which is not solely left to the discretion of the family. Community care and case management expertise anchored by experienced community nurses, allied health professionals and social workers, can provide ongoing health coaching and support (including available access to an out-of-hours hotline). However, out-of-pocket payments are a deterrent, and families need quite a lot of guidance to make good choices, consider the trade-offs (for instance, in the reduction of diaper use by improving continence) and to understand the different financial support schemes available to them.
Social workers or case managers involved in discharge should explore Mdm Siti’s personal support network, relatives, or friends who may be able to assist with different forms of care, such as offering regular respite for Mdm Siti and Enziroh, equipping the home for rehabilitative use, assistance with errands and transportation, and so forth. These personal support options may or may not be available (so that services may need to fill critical gaps), but respecting Mdm Siti involves helping her and her new domestic worker to feel supported and not alone in facing their uncertainties and challenges.
How do we move forward?
Every re-admission brings the patient and their caregivers back to the beginning of the care transition process with opportunities to re-visit what worked, and what did not work. Essentially, if nothing changes, then the cycle will repeat. The key challenge is that our health systems are not seamless − and different patients require different levels of advocacy and support. Moving forward requires patients and their caregivers to be empowered to (a) understand what health problems they have and their healthcare management priorities; (b) set long-term and short-term healthcare goals for themselves; and (c) understand real care planning costs, choices, and sustainable options. Such patient and caregiver empowerment is possible when professionals build up their own capabilities to address the social, financial, and practical issues that make hospital discharges difficult.
Citation
Practice Perspective by Lien, Christopher, ‘Discharge planning’, in Chin, Jacqueline, Nancy Berlinger, Michael C. Dunn, Michael K. Gusmano (eds.), A Singapore Bioethics Casebook, vol. ii: Caring for Older People in an Ageing Society (Singapore: National University of Singapore, 2017), http://www.bioethicscasebook.sg.



